Be built (to last).
The right supplements can help you recover naturally and build a resilient body.

Supplement Quiz
Take this short quiz to discover the perfect supplements for your needs and goals.
About SaltWrap

Built from Broken
Get the best-selling book from SaltWrap founder, Scott Hogan, and start rebuilding today.
The Definitive Guide to Collagen Synthesis: What It Is, Why It Matters, and How to Increase It Naturally
by Scott Hogan, ACE-CPT, COES
Collagen synthesis is a blanket term that describes the process in which your body produces and forms collagen structures.
It’s like muscle protein synthesis, but for your joints.
And just like you can exercise, eat, and supplement to increase protein synthesis (and muscle strength), you can do the same for your connective tissue. To be clear, this is not an article about collagen supplements.
They have a place in this conversation. But the topic of collagen synthesis deserves a much broader discussion that includes the fitness, lifestyle and environmental factors that affect it.
And how that relates to the healing process from injuries, tissue damage, and day-to-day exercise-induced stress.
Though knowledge of the collagen synthesis process provides insight into skin aging, vision and even lung health — we’re going to focus exclusively on connective tissue (e.g. cartilage, tendons, ligaments).
Our goal is to uncover what you can do to boost collagen production and prevent collagen degradation for strong, injury-proof joints.
This article provides a broad-strokes view of the collagen synthesis process and arms you with tactical knowledge of how to leverage it for recovery, injury prevention, and optimal pain-free performance.
Why should you care about collagen synthesis?
Because the degree to which your body produces, forms, and degrades collagen directly impacts:
- injury recovery time
- tissue repair quality
- future injury risk
- mobility and overall joint function
Collagen synthesis doesn’t just matter during the 6-12 weeks you’re recovering from a sprain, strain, or tendinopathy. It dictates the strength and resilience of your joint tissues for a lifetime.
Interestingly, much of what we know about collagen synthesis comes from in-vitro studies (performed on cells in test tubes) and the meat industry, believe it or not.
This is good and bad.
Good because our friends in the meat industry have no vested interest in which supplements you do or don’t buy. They’re simply trying to understand the science behind collagen — and what that means for tissue quality.
On the other hand, animal studies are not as reliable as placebo-controlled human studies.
Luckily for us, the science has advanced leaps and bounds in the last 20 years.
But common knowledge, exercise programming recommendations, and nutrition strategies for optimizing collagen health hasn’t caught up yet.
There's a lot more to collagen synthesis than just taking supplements.
Collagen Synthesis and Soft Tissue Injuries
In high-contact sports like football, soft tissue injuries (muscle, tendon, ligaments, etc.) account for about 70% of visits to physical therapists. Most of those involve connective tissue rather than just muscle, with at least half coming from overuse injuries rather than sudden acute injuries.
According to the Centers for Disease Control (CDC), these figures roughly apply to youth and weekend-warrior adults as well as serious athletes:
- Overuse injuries account for about half of all sports injuries in middle school and high school age students
- Since 2000, there’s been a fivefold increase in the number of shoulder and elbow injuries among youth baseball and softball players
- The parts of the body most frequently injured while engaging in sports and recreation activities were lower extremity (42.0%), upper extremity (30.3%), and head and neck (16.4%)
- More than half of all sports injuries are preventable
Bottom line: improvements in the knowledge and application of joint health management lags behind muscular strength, endurance and performance advancements.
As I’ll explain, this is a big part of the problem.
We’re building bigger, stronger muscles. Faster, more powerful athletes. But we’re doing it on the scaffolding of stiff, injury-prone joint structures.
Soft tissue injuries account for the vast majority of sports, fitness, and lifestyle related injuries. With at least half of those coming from overuse injuries (and likely much more when you consider traumatic injuries that were preceded by gradual breakdown from overuse).
They’re the #1 cause of athletes missing playing time, fitness enthusiasts sitting on the sidelines, and general joint pain in the general population.
Clearly, we need a better way to optimize recovery and prevent soft tissue injuries.
While many sports medicine doctors and physical therapists still cling tightly to the dogmatic approach of anti-inflammatory drugs, rest and ice — the science of collagen synthesis provides insight into how we can do better.
And just in case you’re thinking that you would have heard about this by now if it really mattered, here are a few examples of what you can do to optimize joint health via collagen synthesis:
- A study published in the Scandinavian Journal of Medicine and Science in Sports demonstrated that eccentric exercise (focused on the lowering portion of the movement) increased collagen synthesis rates in soccer players with chronically injured Achilles tendons, and that there is a direct relationship between collagen synthesis and injury recovery in human tendons. This means that people with chronic injuries can use a specific exercise technique to speed up tissue repair.
- Studies show supplementing with Vitamin C after an injury (or when chronic tendinopathy is present) can reduce oxidative stress, help manage inflammation levels, increase bone healing rates, and increase type I collagen synthesis. Vitamin C deficiency leads to collagen structure malformation — suboptimal connective tissue patterns that are weak, stiff and prone to injury.
Preclinical studies demonstrated that vitamin C has the potential to accelerate bone healing after a fracture, increase type I collagen synthesis, and reduce oxidative stress parameters - Orthop J Sports Med.
- In a small placebo-controlled study, 5-15 grams of collagen protein enriched with Vitamin C doubled collagen synthesis versus the placebo group, indicating that this supplement combination coupled with exercises that target at-risk joints has the ability to improve connective tissue strength and prevent injury.
There’s real potential here.
Not just in terms of what supplements to take, but also how (and when) to exercise in a way that bolsters collagen synthesis in injury prone joints, and what lifestyle variables hinder the repair process.
Researchers from respected institutions like The American Journal of Clinical Nutrition and The Gatorade Sports Science Institute have encouraged the leveraging of collagen synthesis for injury repair and joint health maintenance.
If you’re battling through an injury right now, you feel like you’re “injury prone”, or are suffering from joint pain and tendinopathy — understanding and applying the principles behind collagen synthesis can be the difference between getting back to full function, and staying on the sidelines.
In order to understand the collagen production and formation process, we first have to understand what collagen is.
What is collagen?
Despite the typical oversimplified explanations of what collagen is, it’s actually quite a bizarre molecule.
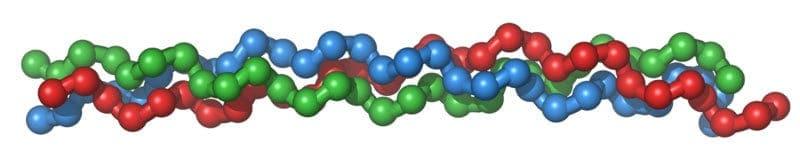
In its natural form, collagen consists of three coiled subunits containing exactly 1050 amino acids. These coils are wound together into a characteristic triple helix structure.
The triple helix image of collagen illustrates how it appears in its natural structural form. Collagen Triple Helix, image generated by the PyMol program, Wikimedia Commons, image rotated 270 degrees
Collagen is the second most abundant substance in the human body (behind water), accounting for about 30% of the total protein in your body.
Its function is to form an extracellular matrix that provides structural support and a mechanism for transmitting force for virtually all organs and soft tissue (including joints).
As you age, your body produces less and less collagen.
By age 60, your ability to produce collagen has decreased by 50%.
This leads to aging joints, saggy skin, and loss of lean muscle tissue.
This is why the collagen supplement industry is booming (despite whether the claims being made by the supplement marketers are substantiated), and why preserving collagen mass in joints and skin is an important part of healthy aging.
What’s the difference between Collagen Type I, II, III, and the rest of them?
There are several types of collagen, but upwards of 90% of the body’s collagen is made up of Types I, II and III.
Most collagen protein supplements are also made up primarily of Types I and III.
Type II collagen (CII) is the primary component of joint cartilage, and the most bioavailable version when taken orally, requiring a much smaller dosage than Types I and III to be effective for improving joint health. Upwards of 90% of your body's extracellular matrix (mix of compounds that provide structural support to joints) is made of Type II collagen.
Is collagen the Holy Grail of Anti-Aging, Fountain of Youth, or Tree of Never-ending Life?
No.
Collagen supplements are not any of those things.
In fact, collagen is an incomplete protein — meaning it doesn’t possess all the amino acids your body needs to maintain health. It should not replace dietary protein.
Plus, most are cheap and not readily absorbed by the body.
Collagen has been grossly over-marketed. It’s popularity is largely based on the fact that low-quality sources are cheap to manufacture, making it a cash cow for supplement companies.
But, there is solid research behind it for supporting joint health and skin elasticity.
Certain types, taken at certain times, do appear to optimize collagen synthesis — especially when combined with other components that allow it retain its natural structure (undenatured). More on this in a second.
++
Now that we have the obligatory “Collagen 101” lesson out of the way, let’s briefly look at the four steps of collagen synthesis.
Each one plays a vital role in the growth, remodeling, and accumulation of collagen.
This is important not just to impress your friends with some esoteric biochemistry knowledge — but also because understanding how different environmental factors affect these four steps gives you insight into building healthy joints.
It provides context into the specific recommendations we make below, and why they work.
What is collagen synthesis?
Collagen synthesis is a blanket term that describes how your body produces, aggregates and forms collagen structures.
It has four distinct processes. Without getting lost in the weeds, here is a quick overview:
🔬 4 Stages of Collagen Synthesis
1. Collagen Biosynthesis — the production of collagen in the body.
Collagen biosynthesis can be likened to the process of making bricks from clay, which will eventually be used for constructing a wall.
Why it matters: Collagen biosynthesis determines how much raw material is produced for your joints to rebuild with, and can be directly influenced by nutrition, exercise, and lifestyle factors.
2. Collagen Cross-linking — the building of connections between collagen molecules to form collagen fibrils (straw-like chains of collagen).
Think of collagen cross-linking in the same way mortar is used to hold bricks together when building a wall. It describes the building of connections.
Why it matters: Heavily cross-linked collagen is more resistant to degradation than less cross-linked collagen. And diet influences this process. For example, animal studies show prolonged low energy diets and low protein diets may interfere with cross-linking. Studies also show that copper deficiency impairs collagen cross-linking, leading to weak formations that are easily irritated and torn.
3. Collagen Fibril Formation — collagen microfibrils are semi-crystalline bundles of collagen.
These fibrils are bundled together like straw into fibril bundles.
Here is where my brick wall metaphor falls apart…
Why it matters: See the image below to get an idea of what collagen fibrils look like once collagen fibers are cross-linked together and bundled. The growth, size, and diameter of these fibrils is influenced by tissue type, age, and stage of development. The composition of these fibrils largely determines how strong, flexible (or stiff) and resistant to degradation the soft tissue is.
4. Collagenolysis — AKA Collagen degradation.
Why it matters: This sounds bad. But it's actually an important physiological process for injury and wound repair.
It kick-starts the remodeling process of suboptimal collagen formations (aka scar tissue), which is necessary not only to repair new injuries, but also to eliminate junky tissue formations from old injuries that have turned into tendinitis or tendinosis.
But like inflammation or oxidative stress, too much collagen degradation causes loss of connective tissue mass. And it’s one of the primary drivers of joint aging and disease.
Collagen degradation doesn’t just happen with aging though. A significant portion (up to 15% in animal studies) of newly synthesized collagen is broken down. This is termed basal degradation. Because such a significant portion of newly formed collagen is lost immediately, this is a key leverage point for improving joint health.
This collagen fibrils image illustrates the straw-like structure that is formed when collagen is cross-linked with adjacent molecules. This image is more "zoomed out" than the molecular structure image of the collagen triple helix illustration above. Fibers of Collagen Type I (edges of image cropped)
How is collagen synthesis measured?
In animal studies and in-vitro (petri dish) studies, collagen synthesis is often measured by amino acid labeling techniques.
For example, animals are given amino acids with distinct signatures that researchers can track, then the total amount of those amino acids that is assimilated into joint structures is used as a measure of collagen synthesis.
Methods like this are problematic, because they don’t take into account collagen degradation rates, and don’t always translate to human joint function.
However, in placebo-controlled environments, methods like this can tell us whether or not an experimental variable (e.g. exercise or a supplement) made a significant impact. And lead us into more relevant human research.
Researchers also measure specific collagen propeptides in human skin before and after wound treatments to determine rates of collagen synthesis.
Blood tests that track collagen propeptides have been used in studies on exercising athletes to measure collagen synthesis as well.
What decreases collagen production and synthesis?
Before worrying about how to boost collagen synthesis, first make sure that you aren’t doing anything to hinder it.
There’s a long list of factors here. Some are out of your control, but you can influence most:
1. NSAID Usage
NSAIDs like ibuprofen and naproxen reduce collagen mass at injury sites, increasing injury rates later by up to 25%.
A study published in the Annals of Physical and Rehabilitation Medicine demonstrated that though NSAIDs effectively relieve joint pain and reduce inflammation in the short term (7 to 14 days), they also delay healing times, increase re-injury rates by up to 25%, and reduce collagen mass at injury sites.
Sports medicine physicians often treat athletes in pain with non-steroidal anti-inflammatory drugs (NSAIDs). However, there is lack of high-quality evidence to guide NSAID use. Their adverse effects have clinical relevance, and their possible negative consequences on the long-term healing process are slowly becoming more obvious....
We do not recommend their use for muscle injuries, bone fractures (also stress fractures) or chronic tendinopathy. from Non-steroidal anti-inflammatory drugs for athletes: an update.
If you take nothing else from this article, remember this:
NSAIDs are not good for your joints long-term.
Especially if you take them regularly.
There are natural alternatives that are just as effective without the side effects.
2. Steroid Hormones (Glucocorticoids, Corticosteroids)
The use of steroid hormones (taken orally) and cortisone injections is a common first line of defense recommendation from doctors and therapists.
While they may help relieve pain and inflammation in the short-term, they have inhibitory effects on collagen synthesis.
Interestingly, this effect has been observed in connective tissue, but not muscles. Indicating that steroid hormones may not be as bad for muscle health, but have long-term negative effects on joint integrity.
Unfortunately the people who benefit most from steroid hormone usage in the short-term (pain relief) are the same individuals who are hurt most in the long-term (failure to repair damaged tissue optimally).
While cortisone injections will temporarily suppress pain and inflammation, they could prolong healing time. If you do get an injection for tendinitis or inflammation, remember that you still have damaged tissue that is susceptible to further injury even if you are not feeling any pain. Avoid heavy lifting for at least one week.
3. Lopsided Exercise Habits
An exercise routine that emphasizes explosive movements like plyometrics and dynamic effort strength training provide a more potent adaptation for muscle than tendons. This results in an imbalance between muscular force potential and tendon resilience, which leads to tendon injuries and tendinopathy.
Young volleyball players, for example, are prone to tendon disorders largely due to the explosive nature of training and competition, and comparatively little amount of movements that are known to trigger tendon adaptations (like isometric exercise and slow movement resistance training).
Simply put, muscles and tendons differ in the types of training they respond to and their timelines for recovery. Understanding these differences is key to establishing balance between muscular force potential and tendon strength and reducing risk of tendon (or muscle) injury. While neglecting to train in ways that boost tendon strength doesn’t necessarily reduce collagen synthesis, it does put you at risk of injury.
Power-dominant training methods like plyometrics increase connective tissue stiffness. Keep reading to learn how adding eccentric-focused exercise to your routine improves tissue remodeling and helps prevent injuries.
4. Disuse (Sedentary Lifestyle)
Disuse leads to a decrease in total collagen in your body, while resistance-focused exercise increases the rate of collagen deposition (formation).
During injury recovery periods, a reduction in activity leads to a reduction in collagen.
Which further increases injury risk. And so the cycle continues.
5. Disease and Genetic Disorders
There are over 200 connective tissue disorders that impact collagen synthesis.
Autoimmune disorders also negatively impact it. Many of these conditions cause the body to attack its own tissues, speeding up collagen degradation.
6. Ultraviolet Radiation (UV Ray) Overexposure
UV rays pertain more to skin health than joint health, but it’s worth mentioning because of the staggering effect on collagen metabolism. According to an article published in the journal Amino Acids, even a one-time exposure decreases collagen in skin. The take home? Avoid tanning beds and get natural sunlight (but don't allow yourself to become sunburnt).
7. Age
Collagen production decreases with age. By age 60, your ability to produce collagen has dropped by around 50%.
8. Hormonal Imbalances
An imbalance of testosterone and estrogen can inhibit collagen synthesis.
Though the research on how estrogen impacts collagen synthesis is conflicting, it appears that low levels of estrogen (especially in aging populations) do inhibit collagen synthesis in joints and skin.
However, too much estrogen also has a detrimental effect on collagen health because it decreases collagen stiffness too much, making it easier for connective tissue to bend and tear.
"Due to the purpose of the tendon in transmitting as well as storing energy, stiffness is a crucial trait in regards to both of these abilities in that it can have a positive effect on both, as long as it does not exceed a certain range of value on either end."
from The effect of estrogen on tendon and ligament metabolism and function.
This means that your tendons and ligaments flourish when there is a balance of stiffness and laxity.
Enough tension to store and transmit energy without bending too much, and enough flexibility to withstand end ranges of motion without tearing.
Likewise, being that testosterone is one of the main anabolic (growth) hormones in the body, having optimal levels helps maintain collagen mass in joint structures.
9. Chronic Inflammation
This is perhaps the biggest misconception around collagen health. Acute inflammation, like you experience right after an injury, is a necessary step for collagen synthesis. It triggers collagen biosynthesis, and helps deliver nutrients to damaged tissue which ultimately leads to collagen formation.
This is yet another reason why blocking inflammation right after an injury is a bad idea.
Problems arise when inflammation is chronically elevated. This can happen in the subsequent weeks after an injury occurs if inflammation levels stay elevated (i.e. tendinitis develops) or if overall systemic inflammation is high for too long.
For example — in osteoarthritis, cartilage destruction and inflammation-mediated type II collagen loss are hallmarks of the condition.
10. Poor Lifestyle Choices
Poor lifestyle choices including bad sleep habits, smoking, and alcohol abuse contribute to increased collagen loss and decreased collagen production.
11. Excessive Caffeine Intake
Drinking a cup of coffee per day likely won't hurt. But caffeine does inhibit collagen synthesis in a dose dependent manner. So pounding energy drinks all day won't help your joints.
12. The Impact of Nutrition on Collagen Synthesis
Diet is the factor you have most control over when it comes to collagen synthesis. While the research on how nutrition affects collagen health doesn’t necessarily deem anything good or bad, it does give us some direction on how to optimize it:
Weight Loss
Reduced calorie diets and corresponding weight loss decreases collagen synthesis.
Low Protein Diets
Animal studies indicate that low protein diets decrease collagen formation, likely from enhanced collagen break-down and impaired collagen cross-linking.
Fasting
An animal study demonstrated that collagen production decreases shortly after fasting begins, and after 96 hours of fasting is reduced by 25% in bone, cartilage and skeletal muscle. This effect is at least partially attributed to the increase in glucocorticoids released by the body during fasting, which have inhibitory effects on collagen synthesis.
Ketogenic and Extreme Low Carb Diets
Insulin and somatomedins (insulin-like growth factors) both stimulate collagen synthesis, indicating that low carb and ketogenic diets could have deleterious effects on collagen mass.
Vitamin & Mineral Deficiencies
A number of vitamins are involved in collagen synthesis. A deficiency in any of these impairs the process:
- Vitamin A (Retinoids)
- Vitamin B1 (Thiamine)
- Vitamin B2 (Riboflavin)
- Vitamin B6 (Pyridoxine)
- Vitamin C
- Vitamin K
- Chromium
- Copper
- Manganese
- Zinc
In sum, just about everything decreases collagen synthesis, right?
Low carb diets do, but so does excess sugar consumption.
NSAIDs and anti-inflammatories decrease collagen synthesis, but then again so does chronic inflammation.
Could I have just summed this article up by saying “all things in moderation..”?
Not exactly. Like most sensible solutions, the answer lies somewhere in the middle of two extremes.
But science also shows us some specific tactics you can employ to beef up your collagen synthesis for strong, supple, injury-proof joints.
7 Ways to Increase Collagen Synthesis
1. Let your body do its job
In response to injury and tissue damage, your body naturally triggers collagen biosynthesis.
You don’t have to do anything to make that happen. Other than get hurt, of course.
In fact, suppressing inflammation too much during the first week after an injury could hinder collagen biosynthesis and nutrient delivery to the tissues that need it most.
Only use ice and pain meds during the first week after injury for pain management or to control excess swelling.
Don’t try to quash inflammation just for the sake of quashing it.
After the first week, keeping inflammation in the healthy range becomes more important for aiding the healing process — especially as you return to normal activities and exercises that could trigger ongoing inflammatory flair ups.
2. Use Heavy Slow Resistance Training (HSR) to boost connective tissue remodeling.
Think about the last time you did a belly flop into a swimming pool.
It didn’t feel good, did it? Belly flops feel more like being smacked with a giant plastic sheet than falling into a liquid pool.
That’s because in response to sudden force water molecules strengthen the tension that connects them, creating a massive surface area capable of knocking the wind out of you.
Now picture yourself standing in the shallow end of the pool.
With one hand, you slowly drag your arm horizontally through the water.
This time, the water acts more like water.
The slow velocity of your hand movement allows the water molecules to move individually, rather than joining forces into a belly-smacking sheet of liquid pain.
This is exactly how collagen fibers in your joints work.
If you lift weights forcefully or move explosively, your connective tissue tenses up into a rigid sheet. And thankfully so. Or your joints would disintegrate every time you move quickly.
But when you move slowly, your connective tissues act more like individual collagen fibers.
This why using slow, deliberate motions while lifting weights helps activate collagen remodeling — breaking apart old junky cross-links, increasing collagen turnover, and allowing your body to rebuild stronger connective tissue structures.
You can put this into your current training schedule by performing 2-3 sets per week of an HSR exercise that targets a weak, or hyper-stiff, joint.
We’ll use the example of performing barbell squats to help support connective tissue remodeling in the hips, knees, and ankles.
At the end of your normal leg workout routine, perform 2 sets of 6-10 repetitions with the following tempo (5/1/5/1):
- Eccentric Phase (lowering the weight): 5 seconds
- Pause in bottom of squat: 1 second
- Concentric Phase (lifting the weight): 5 seconds
- Repeat
Use a weight that’s light enough to control and that doesn’t cause joint pain. Remember, your initial goal with HSR isn’t to build muscle size or strength — it’s to realign and renew connective tissue fibers.
3. Use common sense and moderation when it comes to lifestyle factors.
Avoid smoking, drug use, and high alcohol intake (keep it to 2 drinks or less per day).
Get some natural sunlight, but don’t allow your skin to become red and burned.
Get 7-9 hours of sleep per night.
Limit your intake of NSAIDs and other steroid hormones including cortisone shots. If you must take NSAIDs like ibuprofen and naproxen for an injury or pain, only use them for a week or less before weaning off, or switching to a natural supplement that accomplishes the same goals.
[See Related: Best Practices for NSAID usage]
And eat, move and rest in a way that supports optimal testosterone and estrogen levels.
That includes lifting weights with the intention of building muscle and strength, consuming plenty of protein from testosterone-boosting foods like eggs and grass-fed beef, and avoiding fat gain.
4. Try deep tissue massage and manual therapy.
Just as eccentric-focused exercise supports collagen turnover and remodeling, deep tissue massage can improve collagen synthesis — especially during the mid-term rehabilitation phase of injury recovery (massage is contraindicated during the acute phase of injury, as the body needs time to properly form tissue without further aggravation to damaged collagen structures).
For tendinopathy and sore joints — massage therapy helps break up scar tissue and aid the remodeling process necessary to lay down optimally formed collagen fibers.
Recommendation:
Don’t use deep tissue massage or self-massage techniques in the first 1-2 weeks after an injury. Wait until the initial inflammatory response has subsided.
Do use massage, manual therapy and other mobilization techniques like foam rolling to aid physical therapy efforts and get past nagging joint pains that have become chronic.
5. Whole Body Cryotherapy (WBC)
I honestly didn’t think I would be listing cryotherapy in an article on collagen synthesis and joint health. Sounds like too much a “hack” to be effective
Let’s look at the research on WBC
One 50-person study showed that whole body cryotherapy (WBC) significantly improved pain levels in 78% of subjects. Animal studies show WBC has the ability to suppress inflammation without negatively effecting the collagen remodeling process.
But the jury is still out on the safety and efficacy of whole body cryotherapy.
One study focusing on recovery from musculoskeletal injury showed promise, but researchers weren’t able to clearly outline the mechanisms of action, or even if the perceived improvements in soreness supported long-term functional recovery.
The high cost, many risks (including nerve damage and blood pressure variations) and lack of substantial evidence puts WBC on the fringe.
You’re better off focusing on exercise, deep tissue massage, diet, and the few supplements proven to support collagen synthesis (more on that below).
6. Eat collagen-boosting foods.
When it comes to food, it’s less about finding secret superfoods that boost collagen synthesis, and more about giving your body the basic materials it needs to function properly.
Rule #1 is to eat enough calories. Chronic low calorie diets result in compromised collagen synthesis.
Does that mean you should eat in excess of your caloric needs to make sure your joints are strong?
Hardly.
It does mean that if you are recovering from an injury or tendinitis you shouldn’t follow a strict low calorie diet during that time period.
It’s common for athletes to have spontaneous reductions in calories consumed after an injury occurs. Their overall activity levels have decreased, and their appetite has too.
Many athletes also do this consciously to avoid weight gain.
This can be problematic if their calorie levels drop substantially, and even more so if protein intake decreases.
If you find yourself in this predicament — trying to maintain low body fat levels, muscle mass, and strength following an injury — a good solution is to increase the percentage of protein in your diet. Get more calories from protein, and less from fat and carbs.
By consuming roughly the same amount of protein that you normally would you’ll be protecting muscle mass, which will translate to a shorter path to full recovery.
Here are a few specific foods that give your body the micronutrition it needs to build more collagen:
Citrus Fruits — Vitamin C plays a crucial role in collagen biosynthesis.
Oysters, Shellfish and Seafood — These seafood dishes are rich in zinc and copper — two minerals that support collagen synthesis.
Leafy Greens – Spinach, kale, and other leafy greens are rich in antioxidants like Vitamin A and Vitamin C that support healthy inflammation levels and help regulate enzymes responsible for collagen breakdown.
White Tea & Green Tea — White tea and green tea are believed to help prevent enzyme activity that speeds up collagen degradation, thereby protecting collagen formations.
Along with getting enough protein and avoiding dramatic decreases in calories, add a few of these foods to your plate each week to support overall collagen health
While you could manage with food alone, research shows us that certain food supplements have a significant positive impact on collagen synthesis.
7. Use supplements proven to support collagen synthesis.
Whey Protein
A study published in the Scandinavian Journal of Medicine and Science in Sports demonstrated that subjects who used whey protein isolate along with resistance training saw greater increases in tendon hypertrophy.
Recommended Usage: Consume 30-40 grams per day, ideally within 1 hour of exercising the joints you’d like to bolster.
Vitamin C + Collagen Peptides (primarily collagen types I and III)
An eight-person, placebo controlled study published in the American Journal of Clinical Nutrition showed that taking Vitamin C along with collagen protein (aka collagen peptides) doubled the rate of collagen synthesis in ankle joints compared to placebo. Collagen protein and Vitamin C supplements taken individually also have regenerative benefits when it comes to joints.
Recommended Usage: Take 5-15 grams of collagen protein along with 100-200 mg Vitamin C 30 minutes before exercising a joint that you want to target. In the study referenced, the subjects jumped rope to create exercise-induced stress before measuring collagen synthesis in the ankle joint.
(We created a pre-workout collagen matrix designed specifically for tendon, ligaments, and cartilage. It combines two patented, clinically supported sources of Bioactive Collagen Peptides® with other key nutrients involved in connective tissue metabolism and repair. Learn more here.)
Type II Collagen
A recent study published in HealthMED showed that supplementing with 750 mg of a natural collagen matrix containing collagen Type I, II, V and X can help stimulate collagen synthesis, specifically within cartilage tissues.
That’s why we included this specific collagen matrix in our total joint recovery supplement, Joint Clinic.
Unlike most joint supplements that are designed only to help maintain joint health over time, we formulated Joint Clinic specifically to optimize collagen synthesis and joint recovery.
In addition to the research-backed type II collagen matrix referenced above, Joint Clinic contains two other ingredients that help stimulate collagen production and promote healing:
Curcumin (Turmeric)
In addition to its antioxidant and inflammation modulating benefits, turmeric also supports collagen rebuilding. A 2016 study published in Nutrition Journal described how curcumin has "restored type II collagen and glycosaminoglycan synthesis" in subjects with knee pain.
Joint Clinic uses C3 Complex® Turmeric — with over 100 publications and more than 45 human clinical studies, C3 is the most scientifically-backed turmeric in the world.
Cissus quadrangularis
Known traditionally as the “Bone Setter” plant for its historical use as a recovery remedy for damaged joints and bones — Cissus is one of the few herbs proven to improve joint pain and function in modern athletes.
Joint Clinic contains 1,600 mg of Cissus per serving. This dosages mirrors the active component concentration used in the most relevant study on joint health in athletes.
Grape Seed Extract: Dermal studies indicate that grape seed extract supplementation has a positive effect on collagen deposition during the healing process.
Joint Clinic contains 300 mg of grape seed extract per serving, standardized to 95% polyphenols (active compounds).
Olive Leaf Extract
Olive leaf extract contains a compound called oleuropein that has a protective effect on degradation of collagen and extracellular matrix components. Interestingly, olive and grape seed extract appear to work well when taken together for preventing post-traumatic tissue damage.
Joint Clinic contains 100 mg of olive leaf extract, standardized to 20% oleuropein (active compound).
While there are thousands of supplements available that claim to improve joint health, only a handful are proven to aid collagen synthesis in joint structures.
The nutrients listed here not only help relieve pain and discomfort, but also improve joint integrity.
As far as what to take and when — it really depends on your goals:
-
If you’re looking to speed up and optimize recovery for a nagging joint, I recommend following the TaperSmart Dosage Schedule with Joint Clinic. You can learn more about that here. This method allows you to use maximum clinically-supported dosages for optimal joint recovery during the crucial first few weeks, and weans you off the formula completely in 6 weeks.
-
If you want day-to-day support for collagen synthesis, joint stress and overall joint health — taking 4 capsules of Joint Clinic daily will give you more than enough turmeric, type II collagen, cissus, and other micronutrients like Vitamin C and D that your connective tissue needs for optimal recovery. One bottle will last around 2 months if you take 4 capsules per day.
If you want to increase collagen mass and tissue resilience in a specific joint (i.e. build stronger joint structures), take one serving of Collagen Synthesis immediately prior to exercising the joint you want to strengthen or reduce pain in. Use eccentric-focused training to target the connective tissue you want to strengthen. Then consume 30-40 grams of whey protein within 1 hour of exercising.
Conclusion
Collagen synthesis is one of the most overlooked, underrated processes for helping your joints recover from stress and stay healthy.
Probably because it gets lumped in with the ever-popular “collagen supplement” market.
But as you now know, collagen synthesis is about much more than just powders and pills.
It’s a fundamental process for building and maintaining connective tissue throughout your body.
And fortunately you can influence it through diet, exercise, supplements and lifestyle changes.
Collagen synthesis is a complex process, but your action plan doesn’t have to be.
Here are the best recommendations for improving collagen synthesis that you can implement right now:
Key Takeaways
1. Limit your use of NSAIDs as much as possible. Use natural supplements that help modulate inflammation and pain instead.
2. Glucocorticoids, corticosteroids, and other steroid hormones (whether injectable or in pill form) should be a last resort for resolving tendinopathy and reducing inflammation. Even if your doctor insists on it.
3. Incorporate eccentric-focused exercises into your resistance training routine to help improve collagen remodeling and prevent collagen formations from becoming stiff and injury-prone.
4. Eat healthy, don’t do drugs… you know the drill. Try adding some of the collagen-boosting foods mentioned in this article to your weekly menu.
5. Avoid diets that require extreme calorie restriction, fasting for long periods of time, or excluding macronutrients (that includes both the ketogenic low carb diet and extreme low fat diets).
6. Supplement smart: use a quality collagen supplement like Collagen Synthesis before exercise to help build and maintain cartilage. If you want to support the recovery process, use Joint Clinic to support total joint health.
Whether you have a nagging joint that just won't recover, you feel like your connective tissue can’t keep up, or maybe you are just plagued by overall joint discomfort — optimizing collagen synthesis can help you build and maintain strong, resilient joints.
Founder: Scott Hogan

I created SaltWrap to bring together the most practical ideas in therapeutic sports nutrition, corrective exercise, and functional fitness — with the goal of keeping you (and myself) strong, mobile, and built to last.
I've worked as an A.C.E. Certified Personal Trainer, Orthopedic Exercise Specialist, and nutritional supplement formulator.
But more importantly — I've spent most of my life battling injuries, joint pain, and just being plain beat up. So I know what it's like to struggle toward fitness goals.
SaltWrap is here to push you through injuries, setbacks and perceived physical limitations. To a place beyond what you think you're capable of. Sign up here to stay in the loop.
Learn more about my best-selling injury prevention and recovery book, Built from Broken.